
Office of Environmental Health and Safety
Bloodborne Pathogen Training for Low Risk Personnel
Revised: May 20, 2015
Training Support
This training module must be taken during normal working hours so that you have ready access to Taylor Kriete, Biological Safety Officer. He is available at (504) 952-1337 to answer any questions you have related to this training.
Contents
- Introduction
- Bloodborne Pathogen Information
- Risk Determination
- Exposure Response
- Work Practices

I. Introduction
- Personnel who may encounter blood or body fluids, but not as part of regular job duties, are considered as “low risk” and must complete this training every five years as required by OSHA and State of Louisiana Office of Risk Management.
- This training includes hyperlinks(indicated by red underlined text) to provide you with additional information.
- Click here to view the OSHA standard.

Definitions
- Blood includes human blood, human blood components, and products made from human blood.
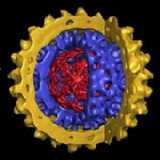
- Bloodborne Pathogens are pathogenic microorganisms present in human blood and other body fluids that can cause disease in humans, including hepatitis B virus (HBV), hepatitis C virus (HCV), and human immunodeficiency virus (HIV).
- Occupational Exposure is reasonably anticipated skin, eye, mucous membrane, or parenteral contact with blood or OPIM that may result from the performance of the employee’s duties.
- Other Potentially Infectious Materials (OPIM) are materials other than human blood that can contain bloodborne pathogens and may potentially be infectious. OPIM include HIV-containing cell or tissue cultures or organ cultures and HIV- or HBV-containing culture medium or other solutions.
Examples of OPIM
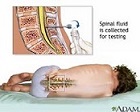
Cerebrospinal, synovial, pleural, amniotic, pericardial, and peritoneal fluids; semen; vaginal secretions.
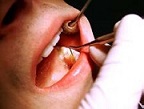
Any material fluid contaminated with blood; saliva in dental procedures.
Bodily fluids in emergency situations that cannot be recognized.
Unfixed human tissues or organs.
Unfixed tissues or organs from HIV- or HBV-infected animals.
HIV or HBV cell cultures or culture medium.
II. Bloodborne Pathogens
Common BBP Diseases
- AIDS is the acquired immunodeficiency syndrome, a serious illness that harms the body's ability to fight infection, and is caused by the HIV virus. Though infected individuals may not initially have symptoms of HIV infection, it may still be possible for them to spread disease.
- Hepatitis B is an infectious illness caused by HBV which causes inflammation of the liver, liver infection, cirrhosis, and liver cancer. Hepatitis B is far more common than HIV and is present in very high concentrations in the blood of infected persons. A vaccination is available for Hepatitis B.
- Hepatitis C is an infectious disease affecting the liver. Symptoms for both HBV and HCV include flu-like illness, jaundice, dark urine, extreme fatigue, nausea, abdominal and joint point, and rash. No vaccine is currently available for Hepatitis C.
Modes of Transmission
- Transmission can be via direct and indirect contact.
- Transmission can occur through:
- Accidental punctures from sharp objects (i.e., needles, broken glass, or other contaminated sharps).
- Contact between broken or damaged skin and infected body fluids (e.g., open sores, cuts, abrasions, acne, or any sort of damaged or broken skin such as blisters).
- Exposure to mucous membranes, eyes, nose, or mouth.
- BBPs are not known to be transmitted across intact skin.
III. Risk Determination
Exposure Risk Determination
Personnel are classified as high risk if they:
- Perform direct patient care activities likely to result in direct or indirect exposure to blood or body fluids.
- Handle human blood, body fluids, tissues or organs.
- Handle equipment, materials or waste that may be contaminated with human blood, body fluids or OPIMs.
- Routinely administer first aid.
- Have potential for to be exposed to blood, body fluids or OPIM in their job duties.
- Examples: Physicians, dentists, laboratory workers, healthcare workers, plumbers and custodial staff, shelter workers, child welfare workers, police officers and others who carry weapons, first responders, firefighters, kitchen staff (that may handle sharp equipment), and public safety workers.
Low risk personnel do not perform any activity listed above (e.g., clerical, administrative staff, IT).
Employee Risk Determination
- The Office of Compliance initially assigns risk levels and associated training for all employees based on job title and department.
- Each supervisor will validate the assigned risk level by reviewing tasks and procedures associated with the employee’s exposure to human blood, body fluids, or OPIMs.
- If the employee’s risk level changes due to supervisory review or the assignment of new tasks, notify the Biological Safety Officer so that the correct training module can be assigned.


Student Risk Determination
- Students enrolled in the Schools of Public Health and Graduate Studies are initially classified as low risk.
- If due to the nature of their work a School of Public Health or Graduate Studies student should in fact be classified as high risk, notify the Biological Safety Officer so that the correct training module can be assigned.
- Since Public Health and Graduate Studies students are not required to be vaccinated for hepatitis B, the “high risk” student will obtain the Hepatitis B vaccination (or verify they are already vaccinated) or complete the Hepatitis B Consent/Declination form (appendix A to the ECP) indicating that they decline the vaccination. Provide the immunization record or signed Consent/Declination form to Student Health.
IV. Exposure Response
Exposure Incident
Exposure Incident: a specific eye, mouth, other mucous membrane, non-intact skin, or a puncture contact with blood or other potentially infectious materials that results from the performance of a person's duties.
For example:
- Needlesticks or scrapes and cuts with contaminated sharps.
- Contact with broken skin through cuts or rashes.
- Splashes to the eyes, nose or mouth.

Exposure Response
The following actions should be taken immediately after exposure:
- Administer first aid. Wash the needlestick or cut with soap and water. Notify your supervisor as soon as feasible.
- If exposure is by splashes or infectious materials to the nose, mouth or eyes, the affected area should be flushed extensively with water, saline or sterile irrigating solution.
- Document the routes of exposure, the biological material of exposure, and how the incident occurred.
- Seek medical attention as soon as possible. HIV prophylaxis is most effective if started within two hours of exposure.
After initial treatment is complete, make an appointment with your healthcare provider as soon as possible for appropriate follow-up.
For more information on exposure response actions, see Section 9 of the Exposure Control Plan .
Post-Treatment Actions
Following an exposure incident, the supervisor must report the incident and complete the appropriate reporting form(s) as outlined in the Incident and Accident Reporting and Investigation Policy .
Counseling for employees and students is available through the Campus Assistance Program (568-8888). The Student Health Clinic can provide access to the Expert Review Panel on behalf of students.
V. Work Practices
Waste Disposal
- Do not handle blood, OPIM or any biological materials without proper training.
- As working knowledge, bioboxes with red biohazard liners are used to dispose of biohazardous waste. Sharps containers are used to dispose of all contaminated sharps (i.e., needles, scalpels).
- All equipment and containers used to store, transport, or ship blood, OPIM or any biological materials must have a label with the word “biohazard” and the biohazard symbol.
- Labels and signs shall be fluorescent orange or orange-red with lettering and symbols in a contrasting color.



Spill Response
Should a incident or spill occur involving blood or OPIM, contact University Police immediately. University Police will notify Environmental Health and Safety to assist in cleaning up the spill.
- Secure the area, keeping all personnel clear of spill.
- Stand by during spill response and cleanup activity to provide information and assistance.
- Refer to the Biological Spill Response Policy for additional spill response guidance.